House Staff Quality Improvement and Patient Safety Conference posters from 2020 to present can be found here.
-

Optimizing Resident Clinic Efficiency Through Process Flow Analysis
Michael Abendroth, MD, MBA; Saumya Copparam, MD; Qiang Zhang, PhD; Rose Costello, MA; Tara Uhler, MD; and Robert Bailey, MD
Abstract
Introduction: Clinic process inefficiencies cause lengthy visit and wait times, which frustrate patients and providers and limit clinic capacity
Objective: To identify process inefficiencies and assess process flow interventions
Methods: Prospective, consecutive series of resident clinic visits over a 3-week period after transferring refraction from tech to resident. Personnel recorded the time spent waiting for and undergoing each clinic process. The clinic also piloted a “Fast Track” from registration to resident for appropriate established patients.
Results: Patients spent 53% of the visit waiting, primarily for the tech. Transferring refraction from tech to resident decreased the wait for tech and tech duration without increasing resident duration. There was no significant reduction in total visit or wait times. “Fast Track” decreased total visit time by 38% but comprised only 3.5% of visits that may have been appropriate.
Conclusion: Reallocating a task from the slowest process decreased that process’s wait and duration but had no effect on total visit or wait times. Process flow analysis identifies inefficiencies and assesses interventions. Automated data collection is crucial for iterations.
-

Improving Emergency Department Efficiency Through Easier Access to Policies
Meryl Abrams, MD; Uma Damle, MD; Adam Brown, DO; Carlos Rodriguez, MD; and Frederick Randolph, MD
Objectives
- We aim to help residents, faculty and auxiliary staff to more easily locate and use institutional clinical policies.
- To improve patient safety by having the institutionally developed policies be more readily available.
-

Analysis of Alert Based Intervention on Management of Hospital-Acquired Acute Kidney Injury: A Prospective Study
Amisha Ahuja, MD; Sonia Bharel, MD; Phil Durney, MD; Goni Katz, MD; Nicholas Tarangelo, MD; James Uricheck, MD; and Randi Zukas, MD
Introduction
The development of acute kidney injury (AKI) during hospitalizations has become a widespread problem that leads to prolonged hospital stays and an increased risk of the development of renal failure. Several national prospective studies have been conducted to identify the most common causes of hospital acquired acute kidney injury (HAAKI) including contrast-induced, drug-induced, sepsis with hypotension, and comorbid organ dysfunction. To attempt to reduce HAAKI and its long-term consequences both to patients and the healthcare system, our study aimed to review creatinine changes among patients admitted to five general medicine teams. Our study goal was to see whether spreading awareness of the common causes of HAAKI through an alert-intervention to providers decreased the rate of occurrence of HAAKI in our hospital system.
-

Reduction of the Duration of Contact Precautions in Patients with a Positive MRSA Swab
Fadi al-Saiegh, MD; Phyllis Flomenberg, MD; Giuliana Labella, RN; Kelli McRory; and James Harrop, MD
Background
Contact precautions (CP) in hospitals are a method of infection control in the transmission of multi-drug resistant organisms. Unfortunately, even though colonization with nasal methicillin-resistant Staphylococcus aureus (MRSA) is common in asymptomatic patients (3.8-4.5%) (6,7), patients are screened for nasal MRSA since it associated with higher morbidity and mortality. However, those who test positive for nasal MRSA are kept on CP even with a cleared MRSA infection(1). At TJUH, patients were kept on CP for 24 months after a positive swab regardless of location. This, unfortunately, led to unintended negative consequences: delay in patient transfer to other facilities (e. g. rehabilitation) (3), lower patient satisfaction (4), decreased health care provider time with patients (5), and increased health care expenditures.
-

Getting Rid Of Stupid Stuff (GROSS) Committee: Residents Dedicated to Streamlining Epic-Related Workflow
Nkosi H. Alvarez, MD; Christina L. Jacovides, MD; Brian M. Till, MD; Walker Lyons, MD; Keyur Patel, MD; Richard Zheng, MD; Adam Johnson, MD; and John Kairys, MD
Objectives
- Identify specific mechanisms for submitting and implementing improvements to the Epic environment
- Standardize high-use order sets
- Incorporate high-value modular components into existing order sets
- Create new order sets to streamline resident workflows
- Improve communication between stakeholders
-

Getting to the Source: Safety Findings in Cervical Cancer Screening Using External Lab Databases
Miranda Aragon, MD; Sunny Lai, MD, MPH; and Geoffrey Mills, MD, PhD
Objective
To investigate the feasibility of using external lab databases to locate Pap smear results completed at outside clinics.
-

A QI Initiative to Reduce Time to Antibiotics in Oncologic Neutropenic Fever
Adam Binder and Jordan Villars
Problem Statement
Neutropenic fever (NF) (defined as temperature of 101o F on one occasion, or 100.4o F sustained over 60 minutes in a patient with an absolute neutrophil count (ANC) less than 500, or suspected drop below 500 within 48 hours) is relatively common oncologic emergency, particularly in hematologic malignancy patients. Expert consensus is that anti-pseudomonas gram-negative antibiotics (abx) should be administered within 60 minutes of detecting neutropenic fever.
At Thomas Jefferson University Hospital (TJUH), internal guidelines for time to treatment in neutropenic fever are in line with expert consensus - 60 minutes. We found that from July 1st – November 21st, 2018 our median time to abx in neutropenic fever cases was 117.5 minutes.
As a result we are proposing to implement a continuous process improvement initiative using PDSA (Plan-Do-Study-Act) cycles with the goal of reducing time to treatment for neutropenic fever.
-

Scanning for QI: Resident and Sonographer Driven Improvement of Radiology Resident Ultrasound Technique
Brian Blumhof, MD; Corinne Wessner, BS, RDMS, RVT; and Kristen McClure, MD
Objective
The aim of this structural QI project is to improve the educational ultrasound curriculum , thus improving overall resident confidence and technical ability in acquiring diagnostic quality sonographic images.
Comparing resident confidence levels and performance against their initial benchmarks as well as against yearly cohorts, we plan to create a long standing addition to the radiology residency at Jefferson, with plans to include additional ultrasound examinations as the curriculum becomes more robust.
Stakeholders include not only the radiology residency, which would benefit from improved resident education and knowledge, but also the hospital and ultimately patients, who stand to benefit from improved delivery of care. Additionally, other residency programs at the hospital can be considered stakeholders, as success of this program raises the possibility of inter departmental educational opportunities.
-

Quality Time: EEG Conference
Nicole Brescia, MD
Background
- Didactic conferences are a defining, common feature of the majority of training programs
- Comprise several hours a week
- Learners and educators from all different levels and backgrounds come together to share experience and knowledge
- Fosters an environment of trust and comradery.
- EEG conferences specifically provide the opportunity to see the perspectives on a study which is sometimes subjective with poor interrater reliability
- Our EEG conference is a recent addition, along with the pediatric epilepsy fellowship, to the AI DuPont Neurology Department
-

Coaching Operating Room to PACU Handoff with a Standardized, Multidisciplinary Checklist
Courtney L. Devin, MD; Kathleen Grife, RN, MS; Marissa Weber, MD; Richard F. Schmidt, MD; Megan P. Lundgren, MD; and Scott W. Cowan, MD
Purpose
To pilot a standardized multidisciplinary bedside handoff for any patient admitted to the post-anesthesia care unit (PACU) from the operating room.
-

Improving Preventive Care in patients with Improving Preventive Care in Patients with Inflammatory Bowel Disease through Use of a Standardized Checklist Tool
Andrew Elden, Richard Denicola, Amy Javia, Raja Dhanekula, Raina Shivashankar, Patricia Kozuch, Stephanie Moleski, and Jorge Prieto
Study Aims
- Improve communication to referring PCP of the preventive care screening needs for IBD patients seen in the ambulatory setting.
- Implement system wide change through the use of a progressively modified EPIC based smart tool integrated directly into our provider notes.
- Increase adherence to guidelines for immunization, cancer screening, infectious screening, osteoporosis screening (DEXA scans), and smoking cessation counseling.
-

Continuity of Care in the Resected Pancreatic Cancer Patient Population at Thomas Jefferson University Hospital
Christian Fernandez, MD; Nazanin Sarpoulaki; Andrew J. Song, MD; and Mark D. Hurwitz, MD
Introduction
- Standard of care for resectable pancreatic cancer according to the National Comprehensive Cancer Network guidelines includes surgery, chemotherapy, and consideration of radiotherapy
- Thomas Jefferson University Hospital is a high volume institution with over 100 surgical pancreatic cancer cases per year
- Adjuvant treatment at high volume centers is recommended at all stages and inpatients at TJUH routinely receive inpatient radiation and medical oncology consultations prior to discharge to discuss the benefit of adjuvant therapies
- Despite these efforts and potential benefit to patients, the rate of follow up and delivery of adjuvant therapies at TJUH have not be characterized
- We retrospectively reviewed patients that received curative surgery at TJUH to assess follow up, adjuvant treatment, and evaluated associated variables
-

Aspiration Pneumonia after Spine Surgery at TJUH
Daniel Franco, MD; Jesse Edwards, MD; Kristen Vogl, PT; Barbara Baskin, SLP; and James Harrop, MD
Problem Definition
Aspiration Pneumonia after Spine Surgery at TJUH has a disproportionately high incidence, compared to other major academic centers When Aspiration Pneumonia is diagnosed in the immediate post operative period, this cascades into increased length of stay, increased overall cost and possibility negative impact for physician and hospital reimbursement At this time, it is unclear which criteria are used by physicians to determine whether an aspiration event has happened.
-

Expedited Referral to Inpatient Hospice Unit Through the Jefferson Methodist Hospital Emergency Department
Brian Fromm, MD and Kory London, MD, FACEP
Background
Palliative care is the branch of healthcare that aims to provide symptomatic relief for patients with chronic or incurable medical conditions. Hospice is a subcategory of palliative care in which the focus is placed on comfort to the exclusion of further curative efforts, generally reserved for patients with a life expectancy of six months or less.
The American College of Emergency Physicians (ACEP) Choosing Wisely guidelines recommend that emergency physicians refer appropriate patients to hospice and palliative services. Preventing hospital admission in favor of transfer to an inpatient hospice unit “can benefit select patients resulting in both improved quality and quantity of life.” [1]
Additionally, from an operational perspective, especially in a system that deals with constant inpatient boarding in the ED, referral to hospice services can prevent acute admissions, opening beds both upstairs and in the ED to other patients. Similarly, CMS penalizes hospitals for return admissions within 30 days for such conditions as COPD/CHF. [2]
The population of South Philadelphia is a diverse group with a large burden of chronic illness. Increasing access to hospice services could allow both greater patient autonomy over their care as well as potentially bending the curve on hospital overcrowding and reducing readmissions.
By December 2018, we aim to institute a system of expedited inpatient hospice referral for patients presenting to our emergency department. Our goal was to increase the utilization of hospice services compared to prior years. Here we examine the initial effectiveness of this system in terms of utilization numbers on a rolling month to month basis.
-

Implementation of a ‘Flow’ Attending Reduces Overall ED Length of Stay in Telehealth Intake Model
R. Fuega, K. Maloney, R. A. Band, B. H. Slovis, K. S. London, and J. L. White
Background
In an effort to improve our efficiency, the Department of Emergency Medicine recently transitioned from an in person physician triage model to a telehealth intake model. With this change, many new gaps have been identified. By uncoupling triage from the in person intake provider, we lost the ability to manage “quick” discharges, to provide secondary oversight of the patients in the internal waiting room, and to directly supervise patients seen in the fast track area. In order to address these new concerns, and to mitigate the loss felt by removing the in person provider from intake, a ‘flow’ attending role was added. Our objective in this study was to determine if the addition of an attending physician for 30 hours per week significantly impacted our patient flow through the department, which we measured primarily using length of stay for discharged patients.
-

Spinal Cord Injury Activation Alert: Revisiting and Revamping Protocols
Ritam Ghosh, MD; Ralph Marino, MD; Michael Wolf, MD; and James S. Harrop, MD
Objective
Our objective was to look at the current protocol for spinal cord injury activation alerts and to highlight deficiencies in the system. Currently, any physician at Jefferson can call this alert, which often leads to a misuse of resources and wrongful identification of true spinal cord injury.
In order to refine the protocol, we believe that the Cord System should be used for the following guidelines:
- Identify patients w Spinal Cord Injury (SCI)
- Identify patients for SCI research trials
- Identify patients who require surgery
-

Application of Alvimopan as a Component of Enhanced Recovery After Surgery (ERAS) Protocol for Patients Undergoing Radical Cystectomy and Diversion (C&D)
Thomas Hardacker, MD, MBA; May Jean Counsilman, MD; Benjamin H. Rudnick, MD; Edouard J. Trabulsi, MD; James R. Mark, MD; Leonard G. Gomella, MD; Mark J. Mann, MD; Costas D. Lallas, MD; and Scott G. Hubosky, MD
Introduction
- Radical cystectomy with urinary diversion (C&D) is performed for patients with muscle-invasive bladder cancer (MIBC) or refractory carcinoma in situ (CIS)
- C&D patients receive one of several types of diversion depending on their age, comorbidities, functional status, and extent of disease (Figure 1)
- Post-operative length of stay (LOS) can be prolonged (9-11 days) and 30 day readmission rates and mortality elevated (30% and 1.5%); return of bowel function usually the rate-limiting step to discharge
- Enhanced Recovery After Surgery (ERAS) protocols utilize pre-, intra-, and postoperative elements in order to improve return of bowel function and decrease LOS
- Alvimopan is a μ-opioid receptor antagonist commonly included in ERAS, and limits deleterious effects of narcotics on the GI system
- The goal of this analysis was to determine the effect of Alvimopan on post-operative LOS and 30 day readmission in patients undergoing C&D
-
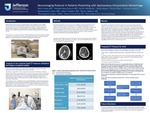
Neuroimaging Protocol in Patients Presenting with Spontaneous Intracerebral Hemorrhage
Kevin Hines, MD; Nikolaos Mouchtouris, MD; Karim Hafazalla; Jacob M. Mazza; Phillip Phan; Giuliana Labella; Muhammad Athar, MD; Adam Flanders, MD; and Pascal Jabbour, MD
Introduction
While lacking evidence based recommendations, most institutions must evaluate spontaneous intracerebral hemorrhages (sICH) for hematoma expansion (HE). If unrecognized, it can be a devastating complication. However, because of the lack of general recommendations for serial imaging, many hospitals, including Thomas Jefferson, have arbitrarily instituted 6 hour an 24 hour stability head CT’s to evaluate for HE.
In our project, we examine the impact of this imaging protocol on the safety and quality of patient care and provide revised recommendations for imaging in sICH at Thomas Jefferson University Hospital and Jefferson Hospital for Neuroscience.
-

Implementation of Standardized Discharge Instructions
Caitlin Hodge, MD; QuyngDiem Lam, MD; Luis A. Mejia, MD; Orlando C. Kirton, MD, FACS, MCCM, FCCP, MBA; Robert Josloff, MD; and Kristin Noonan, MD
Introduction
Previously, same-day surgical discharge instructions were handwritten by residents on generic fill-in-the-blank forms leading to inconsistent discharge instructions. Residents started an initiative to create these standardized discharge instructions. These instructions were designed to improve documentation for post-operative instructions as well as enhance overall patient safety in an attempt to eliminate miscommunications with patients.
-

Improving Glycemic Control and Patient Follow Up in an Uncontrolled Diabetic Population at Jefferson Hospital Ambulatory Practice
Jennifer Hong, MD; Kamal Amer, MD; Sean Clark-Garvey, MD; Rachel Redfield, MD; Timothy Colangelo, MD; Roshni S. Patel, PharmD; and Albert Lee, MD
Aim
- Increase percentage of scheduled follow up appointments in our diabetic population by 50% within 8 months.
- Decrease percentage of uncontrolled diabetics by 10% within 8 months.
-

Improving Residents’ Response Time to Inbox Results
Sean Hurt, MD; Rose Onyeali, MD; and Jason Ojeda, MD
Study Aims
- We aimed to improve the response times to inbox results of the residents and interns at Jefferson Internal Medicine Associates. A standard measure in EPIC is the percentage of inbox results responded to within 24 hours. At the time of project initiation, 50% of all results assigned to resident and intern inboxes were being responded to in this time frame . We aimed to improve this number to 70%
- There is no expectation that residents and interns could respond to all results within 24 hours. Trainee schedules are very crowded, and not all inbox results need to be responded to that quickly.
- We did feel after analyzing this problem, though, that there was significant room for improvement.
-

Escalation of Care After Admission Within 24 Hours
Joseph Jean, MD; Mitchell Berman, MD; Christopher Ponce, MD; and Kory London, MD
Objectives
- Identify high risk patients in the ED who require hospital admission and may need higher levels of care.
- Identify patterns or diagnoses in the ED that predispose patient care to escalations after admission.
-

Evaluation of a Text-Based Event Reporting Process on Resident Event Reporting Rates
R. B. Jones, C. L. Devin, D. Chalikonda, B. Menachem, R. Kanesa-Thasan, K. Klinger, B. Babula, and R. Jaffe
Background
Voluntary event reporting is crucial to identify problem areas in healthcare. At TJUH, resident reporting from July to February during FY19 represented 2% of all report, compared to nursing who accounted for 77% of reports. Resident physicians witness events but do not report them due to cumbersome reporting platform, absence of feedback about reports, lack of reinforcement on how and what to report, and a mindset of not wanting to cause trouble (1,2). Our project aimed to lower the barrier of high administrative reporting burden for residents to report events by creating a HIPAA-compliant, mobile event reporting system.
-

Improving Screening for Diabetic Retinopathy in an Ambulatory Resident Clinic
R. Benson Jones, Guy Katz, Jon Zaid, Navdeep Sangha, and Rebecca Davis
Introduction
While 60% of Americans with diabetes are screened for diabetic retinopathy, the residents in the Jefferson Internal Medicine Associates (JIMA) ambulatory clinic had a lower screening rate (roughly 50%).(1) Our project aimed to increase that screening rate.
-

Developing a Neurosurgical Spine Post-Operative Note Template on EPIC for Improved Multi-Disciplinary Care
Omaditya Khanna, MD; Geoffrey P. Stricsek, MD; Giuliana Labella, RN; James Harrop, MD; and Jesse Edwards, MD
Introduction
The care of neurosurgical spine patients often involves a multi-disciplinary team, including neurosurgery residents, hospitalists, nursing staff, and physical/occupational therapists.
Oftentimes, post-op spine patients are on a non-neurosurgical service (hospitalist, MICU/SICU, medicine), who are provided with scant sign out on the procedure(s) performed.
The treatment team(s) that are helping manage patient care post-operatively are often unaware of the procedure performed, and what are the salient clinical signs/symptoms, radiographic findings, and laboratory values that need to be closely monitored
-

Stopping Clots While Saving Time: Creating an EPIC Index for a Vital Daily Task
Juergen Kloo, MD and Jeffrey Riggio, MD
Introduction
- Appropriate thromboprophylaxis is a pressing issue across the united states and the rate of VTE at Thomas Jefferson University Hospital is higher than hospitals of similar complexity.
- A new tool was created for our EPIC EMR, the VTE Merli Index, that provided at a glance and detailed feedback regarding VTE prophylaxis status
- Prior to implementation of the index, we studied its ease of use. Our goal was to show the tool would decrease the amount of time and number of clicks required to interrogate the EMR for relevant VTE information by at least 50%.
-

We Got the Beat: Improving CPR Quality with Real-Time Metrics
Juergen Kloo, MD; Frances Mae West, MD; and Michael Haviland, RN, BSN
Introduction
High quality chest compressions have been linked to improved survival from sudden cardiac arrest.
The 2015 AHA guidelines recommend the following:
- Rate of compressions between 100 120 CPM
- Depth of compressions between 2 2.4 inches
- Allow full recoil between compressions
- Target CPR fraction at least 60% of the time, ideally 80%
- Avoid hyperventilation
- Collect and use data to improve performance
We set out to show that our clinicians would have a minimum 25% improvement in CPR quality with the use of real time feedback using the new R series ZOLL defibrillators.
-

Implementation of a Volunteer Based Hospital Visitation Program for Older Adults
Mariana R. Kuperman, MD, MPH; Kristine Swartz, MD; Elizabeth Collins, MD; and Jennifer Kim, BS
Background
Hospital Elder Life Program (HELP)¹: a multi faceted, volunteer led, hospital based program has been shown to:
- Reduce the incidence of delirium
- Decrease length of stay
- Reduce hospital costs
Implementation of such a program requires upfront investment.
A smaller, volunteer based visitation program for older adults was started to provide support for the allocation of hospital resources in delirium prevention and establishment of HELP in this institution.
This research aims to investigate the program’s implementation and impact on delirium specific outcomes.
-
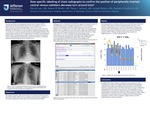
Does Specific Labelling of Chest Radiographs to Confirm the Position of Peripherally Inserted Central Venous Catheters Decrease Turn Around Time?
Patrick Lee, MD; Maansi R. Parekh, MD; Paras Lakhani, MD; Achala Donuru, MD; and Baskaran Sundaram, MD
Objectives
The primary objective of the current study was to decrease the turnaround time (TAT) of PICC CXRs. TAT was defined as the time from completion of the study to finalization of the report by the interpreting radiologist.
-

Reducing Double Chest CT and Unnecesary Radiation: A Quality Improvement Project
Stephan S. Leung, MD; Mansi R. Parekh, MD; Achala Donuru, MD; Paras C. Lakhani, MD; Christopher G. Roth, MD; and Baskaran Sundaram, MD
Objectives
To analyze the variables resulting in double chest CTs being ordered and performed, with the aim to reduce the amount of ordered double chest CTs at Thomas Jefferson University Hospital.
-

Improving Diabetic Retinopathy Screening in a Large Ambulatory Practice
Erica Li, MD; Rebecca Simon, MD; Michael Weissberger, MD; Jennifer Moyer, MD; Rachel Ehrman-Dupre, MD; Andrew Rabovsky, MD; Simon Newsom, MD; Pooja Padgaonkar, MD; Julita Mienko, MD; Sarah Hirsh, MD; and Geoffrey Mills, MD, PhD
Aim 1: To increase the percentage of JFMA diabetic patients with up-to-date retinopathy screening to 60% by April 1, 2019.
Aim 2: To increase the utilization of an in-office portable retinal scanner by identifying current barriers to its use and developing a standardized workflow to overcome these barriers.
Outcome measure: The percentage of adult diabetic patients with a JFMA provider listed as the PCP who have been seen in the Jefferson health system within the last 24 months, who had retinopathy screening once in the last 24 months.
Process measure: The number of retinal scans completed each week.
-

“Can you send over the imaging?” Analyzing the Patient Transfer Process at TJUH
Walker Lyons, MD; Peter Altshuler, MD; Andrew Hallett, MD; Lindsay Lynch, MD; Tommy O'Malley, MD; Steven Woodward, MD; Alicja Zalewski, MD; and Scott Cowan, MD
Objective
Our goal was to investigate possible ways to improve the transition of care when patients are transferred to Jefferson Center City. As a quaternary care hospital with a large transfer volume, it is especially important to look for ways to optimize this process because it can improve timely patient care, reduce and eliminate unnecessary studies and diagnostic tests and save time and work that could be better spent in other aspects of treating the patient.
-

Small Bowel Obstruction: Facilitating Diagnosis and Optimizing Resuscitation and Management
Robin Naples, MD; Kendrick Law, MD; Quinton Campbell, MD; and Ryan Bateman, MD
Introduction
As a common surgical emergency that presents in our Emergency Department, Small Bowel Obstruction (SBO) is a disease process where appropriate treatment relies on early detection, fluid resuscitation, and gastric decompression. Despite SBO representing a common emergency, many patients experience inadequate or delayed management as compared to established guidelines, potentially leading to suboptimal treatment and resolution of SBO. As order sets and alerts within Epic are in place for other disease processes whose management relies on timely diagnosis and fluid resuscitation (e.g. sepsis), objectives for our quality improvement plan involve incorporating elements of alerts and order sets within our EMR to optimize detection, management and resuscitation of patients with small bowel obstruction presenting to the Emergency Department.
-

Lack of Utility and Excess Cost of Routine Perioperative Hematologic Testing in Patients Undergoing Elective Neurosurgical Procedures of the Spine
Lucas Philipp, MD, MPH; Catriona Harrop, MD; David Wyler, MD; and James Harrop, MD
Objective
To prospectively conduct a "mock trial" among 100% (minimum n=200) of elective neurosurgery spine patients to estimate the total projected cost, savings, risk, and feasibility of a redefined/restricted lab testing protocol over the next 12 months
-

Rapid Response Checklists - A Pilot Study for a Novel Approach
Ali Rafiq, MD; Purujit Thacker, MD; and Doron Schneider, MD
Objective
Our goal was to assess residents' ability to think of adequate differential diagnoses in a high-pressure scenario, and their perception of the utility of a checklist during rapid responses.
-

Moisture Chamber for Eye Care after Facial Nerve Injury
Ryan Rimmer, MD; Lauren Bogdan, MD; Gregory Epps, MD; Nikolaus Hjelm, MD; and Erin Reilly, MD
Introduction
- Patients with various lesions of the head and neck may have compromise of facial nerve function.
- Facial nerve (CN VII) has various roles, including movement of facial muscles and, importantly, eye closure.
- When facial nerve is sacrificed or damaged during a surgical cases, steps are often taken intraop to surgically correct the deficit and allow eye closure. However, these patients may not immediately realize the benefit of these interventions.
- In the postop period, appropriate eye care is critical to prevent exposure keratopathy due to inability to close eye.
- Exposure keratopathy is damage to the cornea that occurs primarily due to prolonged exposure of the ocular surface to the outside environment. It can lead to ulceration, microbial keratitis, and permanent vision loss from scarring.
-

It Takes a Village: Developing an Airway Management Bundle to Standardize Emergent Intubation Processes in the Emergency Department
James Sacca, MD; Daniel Casey Kim, MD; and Dimitri Papanagnou, MD, MPH, EdD(c)
Problem Definition
Airway management is at the core of emergent patient care. Emergent intubations in the Emergency Department (ED) at Thomas Jefferson University Hospital (TJUH) have been noted by staff to be variable and not standardized. Staff have also described that equipment tends to be difficult to locate during intubations.
There is no objective data to confirm these claims. Furthermore, there is no bundle in place to guide emergent intubations in the ED.
Our team sought immediate actions to improve ED airway processes.
-

Every Minute Counts: Using Health Information Technology to Reduce Chart Abstraction Times
Christine Schleider, RN, BSN, CNOR; Adam P. Johnson, MD, MPH; Kathleen Shindle, RN, BSN, CCDS; Henry A. Pitt, MD; John R. Kairys, MD; and Scott W. Cowan, MD
-

Creation of an Institutional Toolkit for Evaluation of Multidisciplinary Handoffs
Richard F. Schmidt, MD; Courtney Devin, MD; Nicholas Tarangelo, MD; Andrew Mendelson, MD; Bracken Babula, MD; and Rebecca Jaffe, MD
Objectives
- Create a method for analyzing different handoffs in a variety of clinical settings and scenarios at TJUH.
- Develop a set of standardized survey tools using existing validated language to quantify the perceptions, quality, and needs for different patient care transitions.
- Use results from these tools to cater focused handoff improvement interventions for specific patient care settings.
-

Improving ED Door to Puncture Times for Endovascular Thrombectomy in Acute Ischemic Stroke
Richard F. Schmidt, MD; Nabeel Herial, MD; Robin D'Ambrosio, BSN; Erin Simko, BSN; Fred Rincon, MD; Maria Aini, MD; Pascal Jabbour, MD; Stavropoula Tjoumakaris, MD; M. Reid Gooch, MD; Robert H. Rosenwasswer, MD; and Robin Dharia, MD
Objectives
- Optimize the management of patients presenting to TJUH with AIS who are candidates for ET.
- Enable continued process improvement through improved data collection methods and identification of new process metrics.
-

Improving Postoperative Handoffs in the Neuro-Intensive Care Unit
Richard F. Schmidt, MD; Andrew Mendelson, MD; Sonia Gill, MD; Nicole Hollup, CRNP; Matthew Vibbert, MD; Coleen Vernick, MD; Giuliana Labella, MSN; Marie Wilson, MSN; Caitlin Harley, MSN; Maryanne McCarrin, MSN; Jack Jallo, MD; and Rebecca Jaffe, MD
Introduction
- Transitions of care represent a major source of medical errors, patient morbidity/mortality, and increased healthcare waste.
- 2018 CLER report indicated largely unfavorable responses toward handoffs and care transitions for perioperative services and neurointensive care.
- Use of the IPASS handoff tool is associated with up to 30% reduction in adverse events and 23% reduction in medical errors.
- Implementation of IPASS for postoperative handoffs in the SICU resulted in improved organization, safety, and communication.
-

Expanding Care Access for the Homeless Using Teledermatology
Elizabeth Schoenberg, BA; Nicholas A. Ross, MD; Kathleen McGuinn, MD; Rachelle Lacey, MD; Elizabeth Jones, MD; and Matthew Keller, MD
Aims for Improvement
Specific: Expand dermatology care access to men’s shelters using a teledermatology model enabling us to determine the efficiency, feasibility, and relevance of delivering telehealthcare to the homeless population
Measurable: Surveys to determine patient and provider needs enabling creation of practice guidelines, as well as surveys measuring feasibility and efficacy of the teledermatology intervention
Assignable: JeffHOPE precepting medicine residents, on-call JeffHOPE dermatology residents, dermatology research fellow
Realistic: Pilot two interventions: 1) a teledermatology program to determine feasibility, utility, and efficiency of this care modality in a homeless population 2) a patient-centered practice recommendation booklet to best serve this population including addressing health needs, medicines
Time Based: Run both interventions, simultaneously, for 1 year
-

Initial Response to the Opioid Crisis: Availability of Buprenorphine and Warm Handoff in the ED
Lauren Selame, MD; Benjamin H. Slovis, MD, MA; Theodore Christopher, MD, FACEP; and Kory S. London, MD
Background:
- The United States is in the midst of an opioid crisis.
- The Centers for Disease Control and Prevention has cited Emergency Departments (ED) as important centers for treatment and referral, including medication assisted treatment (MAT), which has been shown to be superior to motivational interviewing and referral alone.1,2
- While direct linkage to outpatient programs via the ED may be an opportunity to better serve this population, data on such “warm handoff” interventions are sparse.
Objective: We initiated an ED opioid use disorder (OUD) pathway, which aimed to initiate buprenorphine therapy and perform warm handoff directly into the community for treatment.
-

Effectiveness of an Educational and Interdisciplinary Intervention in Reducing Continuous Cardiac Monitoring in an Academic Medical Center
Alexander Smith, MD; Rebecca Loh, MD; Philip Margiotta, MD; Bradford Hilson, MD; and Alan Kubey, MD
Smart Aim Statement
- Our study aimed to assess the effect of a combined resident-education-and rounding-checklist-protocol intervention on the percentage of patients discharged with active CCM orders on teaching general medicine services.
- We hypothesized that our intervention would reduce the number of patients discharged on CCM (an estimate of overall inappropriate CCM use) by 50% over a 6-8 week period
-

A Strategy for Noise Reduction to Improve Patient Experiences with Sleep (SNORES)
Vikas Sunder; Eitan Frankel; Neelam Upadhyaya; Merlin Mathew; Ritu Nahar; Michael Brister; Nicholas Young; and Yair Lev, MD
Aim
Our aim was to improve patient-reported sleep satisfaction on the 5 W telemetry unit at Thomas Jefferson University Hospital over a 4 month time period (11/2018 to 2/2019) using a Marpac white noise machine.
-

Time Outs Take Teamwork Improving Patient Safety for Bedside Procedures
Thana Theofanis, MD; Adam Johnson, MD, MPH; Jennifer Harris, MD; Elly Fitzpatrick, RN; Darlene Rosendale, RN; and Rebecca Jaffe, MD
Aims for Improvement
Mission: Improve patient safety through increasing interprofessional collaboration and empowerment in the peri procedural time periods.
Aims
- Increase rate of high quality time outs performed prior to bedside procedures by 50%
- Increase rate of accurate and timely timeout documentation by 50%
-

Treatment Summaries for Head and Neck Cancer Survivors: Improving Patient Self Efficacy and Survivorship Care
Michael C. Topf, MD; Jena Patel; Ramez Philips, MD; and David Cognetti, MD
Objective
- To determine if receiving treatment summaries enhances patient understanding and recall of cancer and treatment details, improves patient self efficacy, and serves as a useful patient tool after completion of head and neck (HNC) therapy
-

Speed and Safety: Emergency Department Ultrasound Lockboxes for Peripheral IV’s
M. Trifan, S. Schiff, D. Devlin, B. Warden, and M. Magee
Objectives
- To decrease the average amount of time needed to place an USGIV by installing lock-boxes with all necessary materials on the ultrasound carts.
- To eliminate a time-consuming step in gathering materials for USGIV, while satisfying safety standards for securing sharps in the department
-

Increasing Awareness for the Opioid Aftercare Coordination Service (OACS)
Michael Weintraub, MD; Harry Wang, MD; Sean Dikdan, MD, MPH; Alexys Monoson, MD; Shalini Krishnasamy; and Jillian Zavodnick, MD
Background
- The United States is in a crisis of opiate related adverse events. From 1999 2017, more than 700,000 people in the U.S. died from drug related overdose; 68% of those involved opioids
- Admissions at Jefferson Hospital for opioid abuse complications are common among the medicine services. Treating patients for their opiate addiction is essential to prevent future opioid overdoses and other complications
- Jefferson has initiated an Opioid Aftercare Coordination Service (OACS) consult system in response to this crisis in order to increase the number of patients who receive medications for opioid use disorder on discharge
- OACS serves both Jefferson Hospital and Methodist and aims to: – Link patients with medications for opioid use disorder after discharge – Provide access to ancillary resources inpatient and outpatient – Provide in hospital counseling
-

The Implementation and Efficacy of a Breast Cancer Wellness Group at Thomas Jefferson University Hospital
Steven Woodward, MD; Peter Altshuler, MD; and Theodore N. Tsangaris, MD
Abstract
Introduction: Breast cancer is not only a physical disease but something that affects our patients’ mental, spiritual, emotional and social wellbeing. There has been literature that demonstrates the positive benefits of exercise, social support, and nonmedical adjuncts for breast cancer patients. There is currently a lack of wellness support within the Jefferson breast cancer community.
Methods: A wellness survey will be distributed throughout the breast surgery and breast oncology clinics to assess the current level of wellness and interest in a breast cancer wellness group at TJUH. This survey will be used both before and after implementation of a wellness group to assess its efficacy within our community.
Results: Pending
Discussion: We believe a breast cancer wellness group will address a major need of support within our Jefferson breast cancer community. This project will not only allow us to meet this need but to assess the basic social, mental, spiritual, and emotional needs of our patients in order to improve our overall patient care.


