-
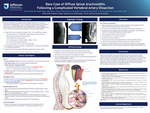
Rare Case of Diffuse Spinal Arachnoiditis Following a Complicated Vertebral Artery Dissection
Elias Atallah, MD; Sophia Dang; Sage Rahm; Nohra Chalouhi, MD; Stavropoula Tjoumakaris MD; Robert H. Rosenwasswer MD; and Pascal Jabbour MD
Spinal arachnoiditis (SA) is an extremely rare and delayed complication of intracranial subarachnoid hemorrhage (SAH). SA is an inflammatory process leading to chronic fibrosis of the spinal cord. Possible pathophysiology is a two-staged disease of initial inflammatory reaction secondary to SAH, followed by a “free interval phase” prior to delayed adhesive phase (i.e. SA). The clinical course can be complicated and is the cause of major morbidity.
-

Prevention and screening of VTE in SCI patients at Thomas Jefferson University Hospital
Erika Dillard, MD, PhD; Yusef Mosley, MD; Joshua Marks, MD; Christina Jacovides, MD; Geoffrey Ouma, MD; and James Harrop, MD
Currently no protocol exists for thromboprophylaxis (TPx) and screening in SCI patients at TJUH. As such, often patients are either not started on TPx or are started on an inappropriate regimen depending on admitting team preference. In addition, patients often receive an admission DUS then weekly thereafter as a screening mechanism for DVT even if asymptomatic.
Our goal is to determine the effectiveness of our current method for initiating pharmacological TPx as well as efficacy and cost of our current screening method compared to national guidelines by addressing these questions:
- What is the occurrence of VTE in SCI patients at TJUH?
- What screening tools are utilized (clinical exam, DUS)?
- How often is recommended LMWH initiated? Does this vary with care team?
- Is TPx initiated within 72h and, if not, why (ie, anticipated surgery, bleeding risk, intracranial hemorrhage)?
- How often are SCI patients screened? How often are clinically insignificant DVTs diagnosed?
- What are the costs associated with the current screening method at TJUH?
-
Comparison of Stroke Cohorts Cared for by Two Different Specialties in a Practice-Based Tele-Stroke Population
Elias Atallah, Kimon Bekelis, Hassan Saad, Ayan Kumar, Justin Turpin, Randa Barsoom, Sophia Dang, Jonathan Li, Stavropoula Tjoumakaris, David Hasan, Maureen DePrince, Giuliana Labella, Robert H. Rosenwasswer, and Pascal Jabbour
Conclusion
- Telemedicine is allowing for more patients suffering from AIS to receive care by dedicated stroke physicians including neurovascular surgeons.
- Our study does not find any difference in outcome between neurologists, who have traditionally managed stroke care, and neurosurgeons.
- Although ischemic stroke is a matter of multidisciplinary management, these surgeons are appropriately knowledgeable to prescribing IVrt-PA and concurrently performing MT in a highly-specialized stroke unit.
-

Cost Savings and Efficiency Realized Decreasing Orders for Type and Crossmatching
Susan Garruto, MSHA, MSN, BSN, RN, APRN, CNOR, RNFA; Katy Loos, MSN, BSN, RN, ACAGNP; and Rae Fierro, RN, CNOR, RNFA
Background
• Thomas Jefferson University Hospital (TJUH) is a Tertiary, Level 1Trauma Center and the Regional Spinal Cord Injury Center of the Delaware Valley with 900+ beds
• C/T Ratio is the ratio of RBC units cross matched for potential transfusion to the number of units actually transfused
• The American Association of Blood Banks (AABB) recommendation for C/T ratio is < 2
• TJUH blood bank, on periodic review by AABB and the College of American Pathologists (CAP) was cited as deficient in C/T ratio quality indicators
• Cost to cross match RBC units is on average $71 with the charge to patient $210
• Cost is built into the Diagnosis-Related Group (DRG), not reimbursed, even when transfused
• Maximum Surgical Blood Ordering System (MSBOS) dictates the RBC units prepared for each surgery. Last revised 2006
• An extra blood bank technician was hired to work 6am to noon tocover the add on CXMs, day of surgery
-

Reorganization of Thalamic Intrinsic Connectivity Following Anterior Temporal Lobectomy
Xiaosong He, Chaitanya Ganne, Michael R. Sperling, Ashwini Sharan, and Joseph I. Tracy
The thalamus has played a crucial role in determining surgical outcome following anterior temporal lobectomy (ATL) in temporal lobe epilepsy (TLE) (He, et al., 2017). Before successfully quantifying the impact of the thalamus on ATL outcomes, this structure’s own intrinsic connectivity must be understood. Accordingly, we characterize thalamic intrinsic connectivity through resting-state fMRI (rsfMRI) longitudinally, exploring its change pre- to post-surgery.
-

Machine Learning Prediction of Seizure Outcome with Presurgical Resting-State fMRI Data
Xiaosong He, Dorian Pustina, Michael R Sperling, Ashwini Sharan, and Joseph I Tracy
Rationale:
Developing a quantitative algorithm for predicting seizure outcome following anterior temporal lobectomy (ATL) in temporal lobe epilepsy (TLE) patient would constitute a significant advance for presurgical decision making. In this project, we tested the ability of topographic properties extracted from presurgical resting-state (rsfMRI) data to predict surgical outcome, using two separate maching learning classification methods (support vector machine, SVM, and random forest RF).
-
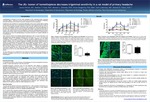
The (R)- isomer of isometheptene decreases trigeminal sensitivity in a rat model of primary headache
Jessica Perino, MS; Nathan T. Fried, PhD; Michael L. Oshinsky, PhD; Bruce Daugherty, PhD, MBA; Seth Lederman, MD; and Melanie B Elliott, PhD
Introduction
Isometheptene is thought to be the active ingredient of the commonly known headache medication, Midrin. Previously, we found only the (R) enantiomer to be effective in alleviating headache behavior in two models of headache compared to the (S) enantiomer.
Experiments using electrical and mechanical stimulation of the dura in animals with no history of head pain have been used to elucidate the mechanisms of the trigeminovascular system at the level of the trigeminal ganglion, trigeminal nucleus caudalis, periaqueductal gray, and the thalamus. The limitation of these acute models is that electrical and mechanical stimulation of the dural blood vessels does not cause long lasting pain similar to recurrent headache pain in humans. Two animal models for the investigation of headache pathophysiology that include aspects of the chronic nature of headache were included in this study. These models provide a new approach to study the pathophysiology of recurrent headache and support validation of novel treatments.
Using behavior methods of monitoring trigeminal allodynia in rats, our group discovered a rat with spontaneous episodic trigeminal allodynia (STA) (Oshinsky et al, 2012). The model was established through 18 generations of inbreeding for testing analgesics and the further understanding of mechanisms of migraine. STA rats experience similar symptoms to human migraine patients, such as episodic trigeminal sensitivity, phonophobia, responsiveness to abortive and prophylactic headache treatments, and sensitivity to migraine triggers. A second well-characterized model of repeated dural inflammatory stimulation (IS), in which an inflammatory stimulant is infused over the dura, also results in persistent headache behavior that has been accepted as a valid model for drug testing. Although the pathological mechanisms between the two models are different, one being considered idiopathic or a spontaneous model and the other inflammatory in nature, the precise mechanism(s) remain elusive.
The aim of this study is to determine the dose response of the (R)-isomer of isometheptene on trigeminal sensitivity in the STA and IS rat models and study the mechanism of action of isometheptene.
Poster presented at: American Headache Society 58th Annual Scientific Meeting in San Diego CA.
-

Rare Case of Metastatic Pituitary Disease
Anitha Somasundaram, MD; Kevin D. Judy, MD; and Kevin Furlong, DO
Background:
Metastatic involvement of the pituitary gland is extremely rare. We present a case of metastatic pituitary disease with panhypopituitarism and diabetes insipidus.
-
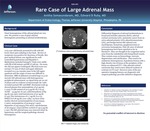
Rare Case of Large Adrenal Mass
Anitha Somasundaram, MD and Edward B. Ruby, MD
Background:
Giant hemangiomas of the adrenal gland are very rare. We present a case of giant adrenal hemangioma presenting as adrenal incidentaloma.
-
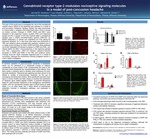
Cannabinoid receptor type-2 modulates nociceptive signaling molecules in a model of post-concussion headache
Jarred M. Stratton, Lan Cheng, Ashley L. Tyburski, Jessica Perino, and Melanie B Elliott
Abstract
The goal of this study was to investigate the role of the cannabinoid receptor type-2 (CB2R) in the trigeminal pain pathway in a model of post-concussion headache. Sprague Dawley rats were randomized to receive either a repeated mild closed head injury (CHI) or served as incision controls. Changes in CGRP, nNOS, and IBA-1 were assessed in the trigeminal nucleus caudalis (TNC) and trigeminal ganglia via IHC. A subset of CHI rats received either a cannabinoid receptor type 2 (CB2R) anti-inflammatory agonist (JWH133), an NSAID (Ketorolac), or vehicle and underwent von Frey testing for trigeminal allodynia. An in vitro brain slice study was performed on TNC and cerebrum slices incubated with capsaicin, capsaicin plus a or media control solutions for 24hrs; CGRP and PGE2 were assessed via ELISA. Repeated CHI showed increases in CGRP and PGE2, and altered nNOS and IBA-1 immunoreactivity in the trigeminal ganglia and TNC, respectively. JWH-133 blocked capsaicin-induced increases in CGRP and PGE2 in the TNC and cerebrum slices. Findings show the CB2R modulates trigeminal pain in a model of concussion, although the mechanisms eliciting analgesia warrant a more in depth investigation.
Poster presented at: American Headache Society in San Diego California.
-
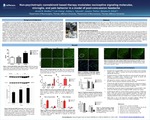
Non-psychotropic cannabinoid based therapy modulates nociceptive signaling molecules, microglia, and pain behavior in a model of post-concussion headache
Jarred M. Stratton, Lan Cheng, Ashley L. Tyburski, Jessica Perino, and Melanie B. Elliott
Background & Objectives
Headache is a common symptom of post-concussion syndrome which may persist in a substantial portion of patients contributing to a poor quality of life and disability. There is a pressing need to develop novel treatments for post-traumatic headache as current treatments have a number of side effects, are contraindicated or lack efficacy. The Elliott laboratory first established models of post-traumatic headache demonstrating sensitization of trigeminal neurons in rodent models of post-traumatic headache using well-known nociceptive and behavioral markers in the pain and migraine fields1-3. Traumatic brain injury in mice increases expression of calcitonin gene related peptide (CGRP) and inducible nitric oxide synthase (iNOS) in the trigeminal pathway, changes that are accompanied by persistent headache behavior, trigeminal allodynia1-3.
The endogenous cannabinoid (eCB) system is a potential therapeutic target for post-traumatic headache. In a series of studies, our laboratory showed CB2R-mediated anti-inflammatory actions in a model of TBI, whereby the reduction of iNOS mRNA and protein and substance P immunoreactivity have implications for headache4-6. The cannabinoid receptor type-2 (CB2R) is an ideal analgesic target as it is devoid of psychoactive properties, shows anti-nociceptive actions upon stimulation, and regulates immune function. What is unclear, is precisely how anti-nociceptive actions are elicited by the CB2R, and if CB2R stimulation will be effective at alleviating trigeminal hypersensitivity in model of post-traumatic concussion or closed head injury. The objective of this study was to determine the role of the CB2R in the trigeminal pain pathway in a model of post-concussion headache, while identifying mechanisms underlying trigeminal pain after mild TBI.
-
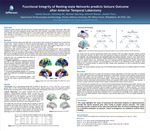
Functional Integrity of Resting-state Networks predicts Seizure Outcome after Anterior Temporal Lobectomy
Gaelle Doucet, Xiaosong He, Michael R. Sperling, Ashwini Sharan MD, and Joseph I. Tracy
Rationale
Predicting seizure outcome (SO) after anterior temporal lobectomy (ATL) is a major clinical goal. With clear evidence that even focal epilepsies disrupt large scale brain networks, resting-state functional connectivity (FC) methods have been increasingly used on a pre-surgical basis to characterize the impact of seizures on brain activity. In this project, we sought to determine whether the functional integrity of resting-state networks (RSNs) prior to surgery can discriminate between patients who obtain good versus poor seizure control after ATL.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


