-

Beyond the Diagnosis: Health-Related Social Needs Screening in Oncology Practice
Rebecca Cammy, LCSW; Munjireen Sifat, PhD; Celeste Vaughan-Briggs, LCSW; Michael Dimino, PhD; and Valerie Csik, MPH
Background
Disparities in cancer care are deeply rooted in social determinants of health, resulting in poorer outcomes for marginalized populations. Health-related social needs (HRSN) screening has emerged as a critical strategy to address these inequities. By identifying and addressing unmet social needs – such as housing instability, food insecurity, and transportation access – we can mitigate barriers to care and improve overall well-being among cancer patients.
-

The Impact of a Cancer Diagnosis on Employment and Finances; Preliminary Findings from a Multi-Site Guaranteed Income Trial
Deidre Geroni, Gregory Garber, Amy Leader, Chiu Yi Tan, Jessica Jacoby, Jason Ma, and Meredith Doherty
Background
A cancer diagnosis affects patients beyond physical health, often disrupting emotional, social, and financial well-being. Employment is central to personal identity, contributing to:
- Financial stability
- A sense of community
- Purpose and fulfillment in daily life
Addressing the impact of cancer on employment is essential to supporting patients' holistic well-being. Despite these challenges, there is a lack of targeted financial interventions aimed at mitigating the disruption to employment, highlighting the need for studies like this one.
-

Whole-Genome Bisulfite Sequencing of Cell-free DNAs Identified Molecular Contributors to Racial Survival Difference in Advanced-Stage Triple-Negative Breast Cancer Patients
Chun Wang, Steven Manobianco, Maria Hafez, Mouadh Barbirou, Grace Qiu, Ashley Wetzel, David Baek, Hushan Yang, and Maysa Abu-Khalaf
Background
- Black women are twice as likely to be diagnosed with triple-negative breast cancer (TNBC) as compared to White women.
- The impact of genomic and molecular factors on the racial disparity in TNBC survival remains understudied.
- Liquid biopsy has yet to be explored in the context of racial survival disparities in TNBC.
-

Social Needs Risk and Patient Outcomes with Supportive Oncology Care
Rebecca Cammy, LCSW and Joshua Banks, MA
Objective
This study utilized social risk data in the electronic heath record collected in routine clinical practice and examined relationships with supportive oncology care contacts and patient outcomes.
-

Addressing Burden in Caregivers of Older Adults with Cancer
Lora Rhodes, LCSW; Kristine Swartz, MD; Caroline Glavin, LSW; Charlotte Zuber; and Kuang-Yi Wen, PhD
Background
Forty-two million adults in the United States are providing unpaid care for a family member or friend over the age of 50. For approximately 2.5 million of these caregivers, cancer is the primary illness or disability of their care recipient (National Alliance for Caregiving and AARP, 2020). As baby boomers continue to age, and the number of cancer survivors continues to increase, the need for informal caregivers will expand exponentially.
While Comprehensive Geriatric Assessment (CGA) is recommended for older patients with cancer and distress screening is recommended for all cancer patients, there are currently no recommendations regarding screening for burden among caregivers. This study was designed to identify factors associated with burden in caregivers of older adults with cancer to better understand the needs of this vulnerable yet often overlooked population.
-
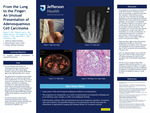
From the Lung to the Finger: An Unusual Presentation of Adenosquamous Cell Carcinoma
Preeti Badve, MD; Sussy Obando Lara, MD; Elisenda Valdez Pena, MD; Myriah Magaris, DO; Zunaira Naeem, MD; Charalambos Solomides, MD; and Avnish Bhatia
Learning Objective
To recognize unusual presentations of metastatic lung disease.
-

Development of an Equitable, Interprofessional Medical Cannabis Education, Certification and Research Program in an NCI-Designated Cancer Center
Gregory Garber, MSW; Jillian Van Sciver, MBA; Denise Young, MSW; Latrisha Bentch, BA; Bracken Babula, MD; and Brooke Worster, MD
Background: Medical cannabis (MC), state-regulated cannabis programs accessible with a physician certification for a qualifying diagnosis, now exist in 47 states. Little attention has been paid to ensuring equitable access to such programs for the most vulnerable cancer patients.1 Estimates of cannabis use in cancer patients range from 30-40%2 yet access to MC is highly dependent on a number of variables including: geography, cost, availability of certifying providers, lack of provider education and a confusing array of state programs coupled with ongoing federal illegality. The historic criminalization of cannabis and the disproportionate impact on People of Color creates another significant barrier. Most state MC programs require patients to have a variety of skills and resources to participate. These may include internet access, email addresses, a credit or debit card, funds to pay for the certifying visit and product and the ability to access a proximal dispensary.
-

Trial in Progress: Sonoporation for Disrupting the Pancreatic Cancer Microenvironment to Enhance Chemotherapy Delivery and Improve Outcomes
James Posey, John R. Eisenbrey, Babar Bashir, Patrick Mille, Atrayee Basu Mallick, Rajan Singla, Spiros Kotopoulis, Ingrid Nordaas, Audun Magerøy Trelsgård, Tæraneh Jouleh, Georg Dimcevski, Odd Helge Gilja, and Flemming Forsberg
Background
- Pancreatic ductal adenocarcinoma (PDAC) is 3% of cancers diagnosed in the United States with 62,210 new cases expected in 2022, but it is the fourth leading cause of cancer-related deaths.
- Hence, there is a considerable clinical need to develop innovative strategies for effective drug delivery and treatment monitoring, resulting in improved outcomes for patients with PDAC.
- Sonoporation is a novel method that can enhance the therapeutic efficacy of co-administered chemotherapy by localized contrastenhanced ultrasound imaging (CEUS) of gas-filled microbubbles (ultrasound contrast agent UCA), which temporarily changes the tumor vascular microenvironment by increasing leakage from angiogenic vessels through microstreaming, shockwaves and the activation of various intracellular signaling responses [1].
- Our Phase I clinical trial of sonoporation in 10 PDAC patients treated with Gemcitabine demonstrated no additional toxicity and an increase in median survival compared to the standard of care treatment (8.9 vs 17.6 months; p = 0.011) [2].
- Subsequent, animal studies investigated 4 commercial UCAs under 2 different acoustic regimes and established the optimal UCA (Sonazoid; GE Healthcare, Oslo, Norway) as well as acoustic settings for sonoporation of PDAC [3].
- There are two major chemotherapeutic regimens for the treatment of non-resectable PDAC, a combination of Leucovorin, Fluorouracil, Irinotecan and Oxaliplatin (FOLFIRINOX), considered the first line treatment, or a combination of Gemcitabine with a nanoparticle formulation of Paclitaxel (Nab-Paclitaxel), the second line treatment. These regiments results in a median overall survival of approximately 11 and 8-9 months.
- The Oncological departments at Jefferson and Haukeland will be responsible for the SoC chemotherapeutic treatment. We will use the hospital’s standard recommended treatment protocols of gemcitabine hydrochloride (Gemkabi®) combined with nanoparticle albumin-bound paclitaxel (Nab-Paclitaxel (Abraxane®)), and FOLFIRINOX.
-

The Impact of Outpatient Supportive Oncology on Cancer Care Cost and Utilization
Brooke Worster, MD; Yifan Zhu, PhD; Gregory Garber, MSW; Sawyer Kieffer, MD; Kyle Cibak; and Aaron Smith-McLallen, PhD
Research Objective
In patients with advanced cancer, interprofessional, non hospital-based care models of palliative care or Supportive Oncology (SO) have been shown in some studies to reduce symptom severity, hospital admissions, and healthcare costs. However, there is little consistency in the composition of SO programs or the degree of integration of social work, nutrition counseling, patient navigation, and nursing care services. There is limited research on quality of care and cost outcomes and current fee-for-service models do not cover the high costs of these non-billable services. We examine the impact of Interprofessional SO care on utilization and medical costs in patients with advanced cancer.
-

The Association of the G8 Questionnaire with Treatment Side Effects and Unscheduled Care Among Older Breast Cancer Patients: A Retrospective Cohort Study
Sameh Gomaa, Louis Cappelli, Kristine Swartz, Tingting Zhan, Andrew Chapman, Ana Maria Lopez, Joseph Lombardo, and Kuang-Yi Wen
Introduction
- Nearly half of the patients diagnosed with breast cancer are ≥ 65 years.
- Older patients with breast cancer are at higher risk for experiencing treatment side effects and unplanned health care.
- This can compromise treatment outcomes and increase the cost of care.
- The G8 is among the most sensitive screening tools for frailty and mortality.
- The aim of this study is to evaluate the association of the G8 questionnaire with treatment side effects and unscheduled care in older breast cancer women.
-

Racial Disparities in Diabetes Mellitus Prevalence in Prostate Cancer Patients on Androgen Deprivation Therapy
Sameh Gomaa; William Kelly, DO; Grace Lu-Yao, PhD; Edith Mitchell, MD; Tingting Zhan, PhD; and Kuang-Yi Wen, PhD
Intro/Background
- Androgen deprivation therapy (ADT) is successfully used in patients with advanced prostate cancer.
- ADT has show to prolong survival.
- The use of ADT is associated with many side effects, most notably an increase in diabetes incidence for patients on ADT.
- African American men have higher prevalence and mortality rates from prostate cancer than White men.
- It is unclear how prostate cancer treatment such as ADT affects these disparities.
- This study examines racial differences in the prevalence of diabetes mellitus in prostate cancer patients based on their ADT status in the US.
-

Smoking and Other Determinants of COVID Severity Among Cancer Patients
Sameh Gomaa; Lindsay Wilde, MD; Tara Rakiewicz; and Kuang-Yi Wen
Introduction
- Cancer patients might be more susceptible to COVID-19 infection.
- With a higher incidence of acute complications, severe disease and higher mortality rates.
- Identifying factors contributing to severe disease remains essential to avoid the risk of severe and often fatal COVID-19 exposure.
- We report on the predisposing factors for severe COVID-19 and increased hospitalization burden in cancer patients at the Sidney Kimmel Cancer Center (SKCC) in Philadelphia.
-

Meaning-Centered Supervision: A Structured Self-Reflection Model to Reconnect with Personal and Professional Meaning in Palliative Care Work
Rebecca Cammy, MSW, LCSW
Meaning-centered supervision explores participant’s sense of meaning of past, present, and future personal and professional experiences. The series aims to reintegrate selfreflection into clinical practice through experiential exercises, homework journaling, and group discussion. Social workers develop a narrative around themes of professional attitude, living and creating work life, and connections with the social work profession. The goal is to help palliative care social workers create a sense meaning and purpose in their work as they develop their personal and professional identities. Additionally, the hope is to support supervisees through any concerns of burnout and compassion fatigue.
-

Early Evidence of Dose-dependent Pharmacodynamic Activity Following Treatment with SY-5609, a Highly Selective and Potent Oral CDK7 Inhibitor, in Patients with Advanced Solid Tumors
Kyriakos P. Papadopoulos, Manish R. Sharma, Erika Hamilton, Debra Richardson, Babar Bashir, Dejan Juric, Geoffrey Shapiro, Graeme Hodgson, Nan Ke, Anthony D'Ippolito, Liv Johannessen, Qing Kang-Fortner, Li Zhou, Maria Rosario, William Zamboni, Hina A. Jolin, Catherine Madigan, Michael J. Kelly, and David A. Roth
-

Breaking the Transportation Barrier: Enhancing Access to Cancer Treatment through Technology and Philanthropy
Rebecca Cammy, MSW, LCSW; Jodi Sandos, MSW, LCSW; and Stephanie Chapman, BS
Cancer patients face many obstacles and challenges after being diagnosed with cancer. Thomas Jefferson University Hospitals’ Sidney Kimmel Cancer Center (SKCC) has effectively eliminated transportation as a barrier to care for patients receiving cancer treatments such as chemotherapy and radiation. SKCC dedicates a full-time patient navigator to assess and connect patients with appropriate transportation resources based on location, insurance coverage, and mobility. The utilization of patient-focused transportation platforms, such as Uber Health, RoundTrip, and Ride Health have streamlined the process, while SKCC philanthropic funds have assisted with associated financial costs. As a result of these resources, oncology patients who would have ordinarily missed appointments due to lack of transportation are now more independent and compliant with cancer treatment.
-

Impact of Palliative Care Consultation on End of Life Care Measures: A Retrospective Analysis of Patients in the Oncology Care Model
Alison Greidinger, MD; Maria Vershvovsky, MD; Evan Lapinsky, MD; Alison Rhoades, MD; Amy Leader, DrPH; Vittorio Maio, PharmD; Jared Minetola; Karen Walsh, MS, MBA; Valerie Csik, MPH, CPPS; and Ruben Rhoades, MD
Introduction
- In 2016 ASCO recommended that patients with advanced cancer receive dedicated palliative care (PC) services1. Early PC involvement is associated with lower spending, fewer 30-day readmission rates, decreased chemotherapy administration at the end of life (EOL) and increased hospice referrals2.
- Many patients are not referred and continue to receive chemotherapy and utilize high-acuity services near the EOL.
- The Oncology Care Model (OCM) is a CMS episode-based alternative payment model promoting high-value care.
- We evaluated the effect of PC visits on EOL outcomes including code status (CS) and spending in the last 30 days of life.
-

Improving the Quality of Patient-Provider Interactions and Promoting Equitable, Accessible and Patient-Centered Cancer Care
C. Vaughan-Briggs, LCSW; A. Petok, LCSW, MPH; T. DeJesse; and Amy Leader, DrPH, MPH
- Philadelphia is among the top 10 cities in the US with populations over 500,000 with a high Community Need Index score (CNI- severity of Health disparity)
- Data from 2015 County Health Ranking, had Philadelphia last of all 67 counties in the state for social economic factors. (unemployment, income inequality, injury deaths, etc. )
- Cancer is a leading cause of mortality in the US
- The SKCC participated in a year-long, externally supported self study to improve the quality of patientprovider interactions and promote more equitable, accessible and patient- centered cancer care. This program aligned with internal initiatives.
- SKCC at Jefferson is NCI-designated cancer center and part of an academic medical center located in Philadelphia. In the catchment area the Incidence and Mortality in 7 out of 10 Major Cancers is higher than state and national averages.
-

Digital Literacy in an Urban Cancer Population: Who Are We Leaving Out?
A. Petok, MSW, MPH; G. Garber, MSW; L. Waldman, BA; A. Leader, PhD; A. Dicker, MD, PhD; and L. Capparella, MSS
Background
- With an increase in and rapid development of health care applications, as well as electronic medical records and patient portals, patients have more access to health information than ever.
- Previous research has found an association between integration of electronic patient reported outcomes (ePROs) with increased survival for patients with metastatic cancer compared to usual care.
- Although greater access to health information as well as personal health records and patient portals can be shown to have positive effects on patient outcomes, the digital divide that is pervasive in the general population extends to oncology as well.
- This project aimed to determine the differences in patient interest in and usage of technology for health care amongst various demographics.
-

Optimizing Psychosocial Care of Older Adults with Cancer: An Early Assessment and Intervention Model
Lora Rhodes, LCSW and Andrew Chapman, DO, FACP
Background
Jefferson Multidisciplinary Senior Adult Oncology Center
History
- Established September 2010
- First multidisciplinary geriatric oncology evaluation center in the tristate area
Demographics
- 890 patients evaluated to date
- All tumor types
- Age 70 and above & Pre-transplant (Bone Marrow) evaluation age 65 and above
Format
- Consultative service
- Two sessions weekly
- Average evaluation time: two hours
Multidisciplinary Team
- Navigator, Medical Oncologist, Geriatrician, Pharmacist, Nutritionist, Social Worker
- As needed: Psychiatry, Rehab Medicine, Radiation Oncology, Surgery
-

Exploring the Role of Life Review Videos with Patients Diagnosed with Advanced Cancer
Lisa M. Capparella, MSS, LCSW, OSW-C and S. Otis-Green, MSW, MA, ACSW, LCSW, OSW-C
Background/Rationale
- Life Review Videos can provide patients with hope, help them finding meaning and value of life.
- Patients with cancer have limited opportunities to discuss their life before cancer.
- Insufficient research related to how patients would want their video to be used by family/friends and who they would chose to share their video with.
- Limited research regarding whether the relationship with the interviewer matters to participants of life review.
-

Safety of Lobar Hepatic Arterial Embolization in Metastatic Uveal Melanoma Patients with Underlying Gilbert's Disease
David C. Feldstein, MD; Robert D. Adamo, MD; Carin F. Gonsalves, MD, FSIR; David J. Eschelman, MS, FSIR; Medical Oncology, Thomas Jefferson University Hospital, Philadelphia, PA; and Takami Sato, MD, PhD
Introduction
❖ Uveal melanoma is the most common primary intraocular malignant tumor in adults.
❖ Up to half of all patients develop systemic metastases, with liver involvement in >90% of patients.1
❖ Various liver-directed, locoregional therapies (i.e. chemoembolization, immunoembolization, radioembolization, and ablation) have played a significant role in prolonging the lives of patients with metastatic uveal melanoma.2
❖ Elevated bilirubin levels are typically considered a relative contraindication for lobar hepatic arterial embolization treatment, given mainly the increased risk of precipitating hepatic failure.
❖ Gilbert's syndrome, also known as benign unconjugated hyperbilirubinemia, is a hereditary disorder of bilirubin conjugation. Gilbert’s syndrome leads to elevated levels of serum bilirubin, that do not truly reflect cholestasis or liver failure and therefore should not exclude patients from targeted embolization therapy.3
Poster presented at: World Conference on Interventional Oncology in Boston MA.
-

Detection of Circulating Tumor Cells in Uveal Melanoma by the Photoacoustic Method
Ryan M. Weight, Shingo Sato, Masahiro Ohara, Mizue Terai, Michael Mastrangelo, Marlana Orloff, Benjamin Goldschmidt, John Viator, and Takami Sato
Abstract
Circulating tumor cells (CTCs) have been shown to be a prognostic marker in breast cancer1. We hypothesize that circulating melanoma cell (CMC) detection could be utilized in the management of uveal melanoma, including early intervention. Prior methodologies for circulating uveal melanoma cell (CUMC) detection have been fraught with poor sensitivity, limiting their clinical utility2. Development of an improved method is necessary to establish the clinical utility of CUMC monitoring. Photoacoustics, also referred to as laser-induced ultrasound, is a novel platform for the detection and capture of CMCs. Photoacoustics uses short duration pulsed light to create ultrasonic acoustic waves in an optically absorbing medium, in this case melanin within melanoma3. As light is absorbed by irradiated chromophores, the optical energy gets converted into kinetic thermal energy trapped within the chromophore and subsequent thermal expansion ensues. Transient thermoelastic expansion of the absorbent cell results in the propagation of ultrasonic acoustic waves which can be detected and analyzed using a piezoelectric response mechanism. In addition, detected CMCs can be isolated by a two-phase flow cell separation technique4. Due to the low cost and melanoma specific capabilities of photoacoustics, we evaluated this technology for the purpose of CUMC detection.
Methods: Cells from uveal melanoma cell line UM002B, established at Thomas Jefferson, were titrated to various cell concentrations and analyzed in a neutral density solution utilizing the photoacoustic method. Uveal melanoma cells of differing concentrations were spiked into isolated healthy donor peripheral blood mononuclear cells (PBMCs) and healthy whole blood samples. PBMC isolates were analyzed for CUMCs.
Results: CUMCs were successfully quantified by the photoacoustic method including single cell detection. Recovery rates of cultured cells in a neutral density solution approached 25%. Recovery rates for CUMCs in whole blood averaged 10% of expected cell yield (56/540 cells detected) with a higher detection rate at lower cell concentrations. Photoacoustics offers a viable method for the detection of CUMCs with an accuracy that meets or exceeds previously reported CUMC yields. Studies analyzing CUMCs from patients with metastatic disease are ongoing.
-
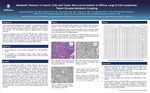
Metabolic Patterns in Cancer Cells and Tumor Micro-environment in Diffuse Large B¬Cell Lymphoma: Tumor–Stromal Metabolic Coupling
Mahasweta Gooptu, MD; Alina E. Dulau Florea, MD; Benjamin E. Leiby, PhD; Barbara Pro, MD; John David Sprandio, Jr. MD; Diana Whitaker-Menezes, PhD; Paolo Cotzia, MD; Guldeep Uppal, MD; Jaime Caro, MD; Jerald Z. Gong, MD; and Ubaldo E. Martinez-Outshoorn, MD
It has previously been suggested that the tumor microenvironment in diffuse large B-cell lymphoma (DLBCL) has prognostic significance. Furthermore, gene expression profiling in DLBCL patients has identified separate subsets with glycolytic and mitochondrial (oxidative phosphorylative) metabolic signatures.
Glycolytic metabolism forms the basis for FDG PET scans, widely used in staging and response assessment in DLBCL. While many assume that the tumor as a whole is primarily glycolytic, the metabolic patterns of cancer cells (C) and surrounding cancer-associated stromal cells (CAS) remain relatively unknown. We investigated the in situ metabolic patterns of C and CAS cells as well as tumor-associated macrophages (TAM) in DLBCL.
-

Prevalence of health-related quality of life (HRQOL) in Asian Americans
Hee-Soon Juon, PhD; Frederic Kim, MS; Seon Yoon Chung, MSN; and Sunmin Lee, ScD
Objectives
To report the prevalence of Health Related Quality of Life (HRQOL) in foreign-born Asian Americans (AA) and to compare this with the general AA from 2010 BRFSS data.
To examine the influential factors associated with HRQOL-4 including English proficiency, perceived racial discrimination, smoking, alcohol use, and sociodemographics.
Background
Quality of life (QOL) represents individuals’ subjective perception of multidimensional aspects of life including physical, psychological, social and spiritual aspects.
HRQOL represents the physical and mental health domain of QOL.
Centers for Disease Control and Prevention (CDC) has been measuring HRQOL to capture people’s overall perceptions about their health; HRQOL has become an important component of health surveillance (U.S. DHHS, 2000).
While acculturation and racial discrimination have been negatively associated to the number of chronic health conditions and well-being of AA, their influence on HRQOL has not been studied.
Public surveillance study has typically considered Asian Americans as a single group and little is known about how HRQOL and health-related risk factors vary among foreign-born Asian Americans including Chinese-, Korean-, and Vietnamese- Americans.
Poster presented at APHA in Chicago Illinois.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


