-
60 Year Old Male with Autonomic Dysreflexia in C7 AIS A secondary to a Suprapubic Catheter Inflation in the Membranous Urethra
Brandon Kase, MD; Joshua Levin, DO; and Kristin Gustafson, DO
Introduction: Autonomic dysreflexia is a potentially lifethreatening complication in patients with a spinal cord injury above the level of T6. A dangerous symptom is an increase in blood pressure induced by reflex sympathetic hyperactivity secondary to a noxious stimuli which can lead to cerebral hemorrhages, seizures, heart failure or pulmonary edema.1 The most common causes of autonomic dysreflexia are noxious stimuli to the 1) bladder such as urinary tract infection, distension, or catheterization; 2) bowel, such as constipation or 3) skin such as wounds, or tight clothing. Though Foley catheters and intermittent catheterizations are well known causes of dysreflexia there is little literature about suprapubic catheters inappropriately inflated causing autonomic dysreflexia.2
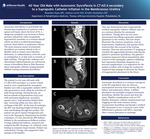
Case Description: The patient is a 60-year-old male with C7 AIS A SCI secondary to a motor vehicle crash in 2021 complicated by neurogenic bladder now with a suprapubic catheter (SPC) who presented to acute rehab for activities of daily living training. During his stay, he had an episode of hypertension (233/109) with associated diaphoresis, increased spasms and a “cold sensation behind [his] legs” occurring within one hour after an exchange of his SPC. At the time of exchange, the SPC was draining bright red blood and clots and flushing through the urethra. The patient was given topical nitroglycerin and sent to the Emergency Department for further evaluation. CT scan showed the SPC balloon inflated in the membranous/bulbous urethra. Urology deflated the balloon, retracted and replaced the SPC draining 1.2L of bloody urine leading to symptom improvement. Patient was evaluated by Urology who suspected a false passage in his bladder.
Discussion: This case demonstrates how inappropriate urethral suprapubic catheter inflation may act as a noxious stimulus for autonomic dysreflexia. Though there are few cases documented describing suprapubic catheter placement in the urethra; this case clearly illustrates the common symptoms, such as hypertension, diaphoresis, and spasms which resolved after the reversal of the inciting stimulus. This case also provides CT imaging to visualize the aggravating stimulus inducing the patient’s autonomic dysreflexia. The patient’s symptoms improved almost immediately after removal of the suprapubic catheter exhibiting how important immediate diagnosis is to prevent complications. It is imperative for the patient to follow with Urology for workup for suspected false passage to decrease the chance of inappropriate placement in the future.
Conclusion: Autonomic dysreflexia is a common emergency in the SCI population that can often go unrecognized and may lead to stroke, MI, renal failure, and pulmonary edema. A skilled physiatrist can promptly recognize autonomic dysreflexia, identify the source and treat the cause. Bladder complications such as UTI, bladder distension, catheter misplacement and clogging are the most common causes of autonomic dysreflexia and though a urethral SPC placement is rare, it must be a part of the differential in patients with SPCs, especially after a recent placement or exchange.
-
Steroid Treatment Causes Weakness in Spinal Dural Arteriovenous Fistula
Mina Na, DO; Brandon Kase, MD; Roger Liu, DO; and Kristin Gustafson, DO
Introduction: Spinal dural arteriovenous fistula (SDAVF) is an abnormal connection between the arterial and venous system creating an increase in blood flow and pressure into the spinal veins1 at an estimated frequency of 5-10 cases per million per year.2 Activities that increase intrathoracic and venous pressure such as Valsalva, abdominal compression and steroids2 can lead to a venous infarction, subarachnoid hemorrhage, paraplegia or tetraplegia.3 SDAVF is difficult to diagnose as it presents similarly to other neurologic disorders, but if diagnosed early, deficits can be prevented and reversed with intervention.1
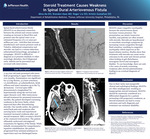
Case Description: A 54-year-old male presented with lower limb progressing to upper limb weakness over months. Examination was significant for 2/5 hip flexion, 3/5 knee extension, 1/5 dorsiflexion, 4/5 plantarflexion, brisk reflexes and intact sensation up to the T4 dermatome. Cervical spine MRI demonstrated a longitudinal T2 hyperintensity along the cervical and upper thoracic cord. After intravenous steroid treatment for presumed transverse myelitis, the patient developed worsening weakness in the lower limbs, which improved days after discontinuing steroids. One month earlier, the patient noted back pain and weakness after carrying heavy tools and experienced transient increased weakness after oral steroid treatment. MRA revealed a SDAVF at the craniocervical junction. The patient ultimately underwent retrosigmoid craniotomy for ligation of the fistula. While initially recommended for comprehensive inpatient rehabilitation, the patient progressed from minimal assistance to supervision and was discharged home.
Discussion: SDAVFs cause congestive myelopathy because the arteriovenous shunt increases venous pressure. The presentation can mimic transverse myelitis, and patients are often treated with steroids. Steroids are hypothesized to exacerbate neurologic symptoms by increasing venous congestion through fluid retention, resulting in congestive myelopathy which improves as the hypervolemia resolves. Studies show that treatment with steroids can cause worse outcomes in the acute and chronic period when looking at gait disturbance, neurogenic bowel and neurogenic bladder. To our knowledge, there are only a few cases of acutely worsening weakness after steroid administration leading to an eventual diagnosis of SDAVF.
Conclusion: Due to their rarity and nonspecific clinical and radiological findings, SDAVFs are often misdiagnosed, resulting in inappropriate steroid treatment. SDAVFs should be cautiously considered as a differential diagnosis for a patient presenting with progressive weakness, as steroid treatment can lead to worse outcomes and early diagnosis and treatment can minimize disability.
-

Upper Limb Capabilities, Self-Care and Fine Motor Activities with and Without Equipment in Persons with Cervical Spinal Cord Injury at Discharge from Rehabilitation and 1 Year Post-Injury
Ralph J. Marino, David Chen, Sara Mulroy, Edelle Field-Fote, and Benjamin Leiby
Introduction: There is little information on the impact of assistive technology or devices (AT) on function. The purpose of this project was to explore the impact of AT on self-care (SC) and fine motor (FM) function in persons with cervical SCI, and to examine the functional capabilities of those who benefit from AT.
Methods: Persons with acute cervical SCI, all levels and AIS grades, with an upper extremity motor score (UEMS) > 0 were enrolled. At discharge from rehabilitation and 1 year post-injury we collected the Capabilities of Upper Extremity questionnaire (CUE-Q), and the combined SC and FM questions of the SCI Functional Index (SCI-FI) and SCI-FI/AT short forms. The arm with the highest CUE-Q side score was designated the better side. The impact of AT on SC and FM function was evaluated by looking at the difference in SCI-FI and SCI-FI/AT scores, and changes over time.
Results: There were 67 participants with data at rehab discharge and 1-year post-injury, 50 male and 17 female, average age 43.3 ± 15.6 years.
- Median scores by neurologic groupings are shown in the table. All groups demonstrated improvements in CUE-Q and SCI-FI scores from discharge to 1 year post-injury (table and radar charts).
- By neurologic group, AT was useful for the greatest percentage of persons classified as C4-C5 AB for FM and C6-T1 AB for SC), least useful for C6-T1 CD (charts at right).
- AT was helpful for the greatest number of items for SC in the C4-C5 CD group at discharge (bolded numbers in table).
- There tended to be less use of AT for tasks at 1 year compared to rehab discharge. For example, the percentage of persons using AT for brushing teeth at discharge was 48%, while at 1 year it was only 25%.
Conclusion: Many persons with tetraplegia are able to perform self-care and fine motor tasks easier using AT, but the benefit depends on the level and severity of injury. There is a decreased reliance on AT over time, which may in part be due to continued recovery after rehabilitation discharge.
-
Carbidopa-Levadopa Improves Speech Apraxia After Open Traumatic Brain Injury
James J. Bresnahan, MD; Philip J. Koehler III, DO; and Mithra B. Maneyapanda, MD
Case Description
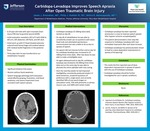
- A 24-year-old male with open traumatic brain injury (TBI) due to gunshot wound (GSW).
- Initial evaluation revealed a GCS of 3 with GSW to left arm, left abdomen, left flank, and left skull.
- Initial work up with CT-Head showed extensive subarachnoid hemorrhage and cerebral edema with residual bullet fragments in the posterior fossa.
- Thirty days later he was transferred to our rehabilitation hospital.
-

An Unusual Cause of Proximal Thigh Pain: Focal Dystonia of the Psoas
James J. Bresnahan, MD and Mitchell H. Paulin, MD
Case Description
- 68-year old female presented for evaluation of right groin pain.
- The pain in her groin radiated superiorly to the lower abdomen and inferiorly to the anteromedial aspect of the proximal thigh and was ongoing for >8 years
- Physicians seen: Neurosurgery, Orthopaedics, Pain Management
- Testing: MRI L-Spine showing degenerative changes and no significant neuroforaminal or spinal stenosis.
- Treatments: PT, multiple epidural steroid injections, facet joint injections, medial branch blocks, and a spinal cord stimulator trial
-
Locked-In Syndrome Due to Neuromyelitis Optica Spectrum Disorder in Acute Rehabilitation: A Case Report
James J. Bresnahan, MD; Summer Schultz, MD; and Mithra B. Maneyapanda, MD
Case Description
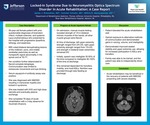
- 56-year-old female patient with prior questionable diagnoses of brainstem infarct, multiple sclerosis, and systemic lupus erythematosus who presented to the hospital with progressive dysarthria, lethargy, and weakness.
- MRI noted bilateral demyelinating lesions of the midbrain, pons, and middle cerebellar peduncles as well as nonspecific signal abnormality in the spinal cord at T6-T7.
- Her condition further deteriorated to flaccid complete tetraplegia. Communication was limited to extraocular movements and eye blinking.
- Serum aquaporin-4 antibody assay was positive.
- She was diagnosed with NMOSD resulting in transverse myelitis and locked-in syndrome.
- She was treated with IVIG and high-dose steroids and eventually plasma exchange.
- She completed 76 days of acute rehabilitation with a 3-day absence for rituximab infusions.
-

A novel case based approach to ICF education for PM&R residents
Nick Freedman, DO; Michael Mallow, MD; and Nethra S. Ankam, MD
Little exists in the literature on reliable methods of ICF education. Our goal was to increase knowledge of the ICF and encourage residents to use the ICF framework to inform their clinical thinking through a case-based exercise.
-

Trends in Rates of ASIA Impairment Scale Conversion in Traumatic Complete Spinal Cord Injury
R. Marino, M. Leff, D. Cardenas, D. Chen, S. Kirshblum, and B. Leiby
Objective: Recent studies on conversion of ASIA Impairment Scale (AIS) grades report higher rates of conversion than older studies. The purpose of this study is to examine the rate of conversion over time in persons with ASIA Impairment Scale (AIS) grade A spinal cord injury (SCI), accounting for level of injury.
Methods: Subjects were injured between 1995 and 2015, enrolled in the National SCI Database as Day-1 admissions, at least 16 years old at the time of injury, classified as AIS A, and had an initial examination within 2 weeks of injury. Change in AIS grade was determined for subjects who had followup examinations at least 30 days post injury. Subjects were grouped in 3-year intervals and trends in AIS grade conversion were assessed for the total sample and by tetraplegia (Tetra), high paraplegia (T1-9, HPara) and low paraplegia (T10-12, LPara).
Results: There were 2037 subjects with usable initial examination data, of whom 1877 had a follow up examination. Average age at injury was 35.0 +/-15.4 years, 79.8% were male, 44.6% Tetra, 35.3% HPara, 20.1% LPara. Overall 80.8% remained AIS A at follow-up, with 8.8% converting to motor incomplete. Change in AIS grade differed by level of injury: 71.4%, 90.9% and 83,2% of Tetra, HParaand LPararemained AIS A, with 13.5%, 4.5% and 6.1% respectively converting to motor incomplete. There was a strong trend towards increased rates of conversion over time, especially for persons with Tetra (p<0.01 for all groups). For Tetra, conversion rates to incomplete (AIS B-E) were 17.6% in the 1995-1997 period increasing to 50% in the 2013-2015 period, while conversion rates to motor incomplete (AIS C-E) were 9.4% increasing to 28.1% at these times. For Hparaover the same periods conversion rates to incomplete changed from 5.3% to 17.6% and to motor incomplete from 3.0% to 6.8%. LParaconversion rates to incomplete changed from 8.0% to 23.1% and to motor incomplete from 2.7% to 15.4%.
Conclusion: Although there is some variability in rates, conversion from complete to incomplete or motor incomplete has been increasing over time, particularly for persons with tetraplegia.
-

Functional Swallow-Related Outcomes Following Transoral Robotic Surgery for Base of Tongue Carcinoma: A Pilot Study
Kelly Salmon, SLPD, CCC-SLP, BCS-S, CLT-LANA and Cesar Ruiz, SLPD, CCC-SLP, BCS-S
In an era where the incidence of oropharyngeal cancer has been growing steadily, there is a limited amount of research exploring functional outcomes for individuals whose definitive cancer management approach includes transoral robotic surgical (TORS) resection with or without adjuvant treatment.
This study was designed to examine functional outcome measures related to tongue strength, swallow function, oral intake, and quality of life in individuals newly diagnosed with base of tongue (BOT) cancer whose treatment plan included surgical resection via TORS, with or without a plan for subsequent adjuvant treatment in the form of radiation or chemoradiation. Data was collected preoperatively and at several time points postoperatively.
The purpose of this study was to determine whether TORS resection for early-stage BOT SCCA affected: (a) lingual strength, (b) swallow safety and efficiency, (c) oral intake, and (d) swallowing-related quality of life.
-

A Week Devoted to Wellness in the Preclinical Phase: Lessons Learned
Nethra S. Ankam, MD
Background
During the 2017-2018 academic year, a large private medical college underwent a complete transformation of its curriculum from a primarily lecture based, traditional format to an integrated, longitudinal format that included both time limited blocks and longitudinal threads of content. Wellness, conceptualized at both wellness of the provider and the patient, is one of the eight threads.
Goals
- Provide a structured pause in medical school for you to reflect on your own wellness
- Allow time to explore the ideas of resilience
- Provide time for rejuvenation
- Allow you to start building productive habits to last you throughout your entire medical careers
-

Culture of Mobility
Beth Colborn, DPT; Helene Daly, MSN, RN; Kathleen Hilbert, RN, MSN, CM; Gordon R. Reeves, MD; Jessica Shank, PT, MPT; Elizabeth Singh, DPT; and Lisa Wus, DNP, RN, CRNP, PCCN-CMC
Objectives
•Create an interdisciplinary approach to patient mobility and functional independence
•Provide education and support to lead a culture of mobility
•Develop a system that reduces immobility related adverse outcomes and promotes overall patient well-being
•Utilize evidence based practice to create a program that will decrease variation in patient care in order to optimize hospital based outcomes
-

All Limbs Lead to the Trunk
Daniel E. Graves, PhD and Darryn Atkinson, PhD, PT
This poster describes the development of and the psychometric properties of the trunk scale that measures the voluntary motor ability in the thoracic and upper lumbar regions. The function of the trunk musculature has far reaching implications, particularly in persons with SCI, where postural control and voluntary movement are compromised to varying degrees. Precisely coordinated muscle actions must occur in the appropriate sequence, duration, and combination for the optimal movement function and maintenance of balance and posture during dynamic activities. Trunk mobility is required for nearly all mobility tasks, particularly transitional movements such as rolling, supine to sit, and sit to stand, as well as activities of daily living which involve upper extremity movements such as reaching. The muscles innervated by the thoracic and lumbar spine play key roles in body positioning and posture which are very important in conducting functional activities such as ambulation, reaching and activities of daily living (ADL)1.
Poster presented at: ISCOS Annual Meeting in Dublin Ireland.
-
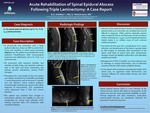
Acute Rehabilitation of Spinal Epidural Abscess Following Triple Laminectomy: A Case Report
B. A. Dahlben, MS and D. Fleischmann, MD
Case Description:
- A 36-year-old man presented with a large epidural collection, shown on MRI to extend from C1-S5 and resulting in spinal canal narrowing (Figures 1-3). The patient was admitted for acute inpatient rehabilitation after neurosurgical treatment and stabilization s/p C7-T1, T7-8, L4-5 laminectomies.
- He presented with impaired mobility and activities of daily living, and reported moderate pain in the back and lower extremities, but without specific distribution, during PT/OT therapies.
- Throughout his 7-day length of stay, the patient was closely monitored for methicillin-susceptible S. aureus bacteremia, and he received IV oxacillin and oral rifampin. Active medical problems included bright red blood per rectum with a likely diagnosis of hemorrhoids, DVT prophylaxis, newly diagnosed Type 2 DM, and urinary retention.
- The patient was switched from straight to intermittent catheter, but inability to void was complicated by urinary tract infection (UTI). Voiding improved after UTI treatment with macrobid antibiotic.
-

Road to Recovery: Dysphagia Treatment With An Adult with SMA Type II
Kara Maharay, M.S., CCC-SLP, BCS-S; Kelly Salmon, M.A., CCC-SLP, BCS-S, CLT-LANA; and Ronald S. Kaiser, Ph.D
Objective: Spinal Muscular Atrophy (SMA) is a genetic and degenerative motor neuron disease that affects muscle control including the muscles responsible for head and neck control and swallowing (Kesting, n. d.). There is limited research on the benefits of exercise as a therapeutic modality for people with Spinal Muscular Atrophy (SMA) (Swoboda et al., 2007) and no existing research specifically targeting pharyngeal or laryngeal strengthening to improve swallow function. As demonstrated by the positive outcome in this case study, speech-language pathologists should be aware that various modalities for dysphagia treatment such as biofeedback, neuromuscular electrical stimulation (NMES), and an exercise based approach in conjunction with compensatory strategies may be effective in the swallowing rehabilitation of patients with patients with SMA.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.



